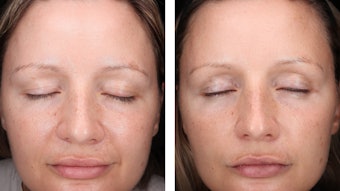
Acne is an inflammatory skin disease that, for individuals afflicted by it, can leave both physical and emotional scars. While acne is most often thought of as the terrible and inevitable bane of late adolescence, it can just as easily become a chronic problem for adults. In fact, acne is considered to be the eighth most prominent disease in the world, impacting nearly 10% of people (adults and adolescents) on a global scale1 and more than 80% of adolescents in developed countries.2
Log in to view the full article
Acne is an inflammatory skin disease that, for individuals afflicted by it, can leave both physical and emotional scars. While acne is most often thought of as the terrible and inevitable bane of late adolescence, it can just as easily become a chronic problem for adults. In fact, acne is considered to be the eighth most prominent disease in the world, impacting nearly 10% of people (adults and adolescents) on a global scale1 and more than 80% of adolescents in developed countries.2
While acne itself is not normally considered to be a life-threatening disease, the social impact of acne can be utterly devastating; significant increases in depression and anxiety in acne sufferers can lead to a severe decline in quality of life.3 Considering how emotionally damaging the effects of this widespread disease can be, it is little wonder why the skin care industry has a strong interest in developing products to counter the effects of this dreaded skin condition.
In vitro Approaches to Anti-acne Testing
Acne is thought to be caused by an infection of the pilosebaceous unit by the Propionibacterium acnes (P. acnes) bacteria. The condition preferentially impacts areas of the skin with a high density of sebaceous glands, such as the face, back and chest. In general terms, acne is characterized by four major pathogenic factors, and in order for a material to be effective at treating acne, it should target one or more of them; these include:4
- Localized skin inflammation;
- An increase in sebum production by sebocytes;
- Keratinocyte hyperproliferation; and
- An overgrowth of the P. acnes bacteria.
Skin Inflammation
The epidermal layer of skin essentially forms the first layer of defense between our bodies and the outside world. While the skin contains immune-specific cells, such as Langerhans, other types of non-immune-specific cells also possess an innate immune ability and can recognize microbial invasions. With respect to acne, the epidermal cells with innate immune ability to recognize and respond to the problematic P. acnes are the keratinocytes and sebocytes. This recognition is thought to occur through a specialized membrane protein found on these cells belonging to the Toll-like receptor (TLR) class of proteins.
The TLR family is a remarkable family of proteins designed to respond to various sorts of stimuli associated with bacterial, fungal and viral infection. Members of this family can respond to lipopolysaccharides from Gram-negative bacteria, unmethylated CpG DNA or ssRNA associated with viruses, bacterial specific ribosomal subunits and a host of other microbial components.5 With respect to how keratinocytes and sebocytes recognize P. acnes, this identification is thought to occur via TLR2, which recognizes peptidoglycan, a component of Gram-positive bacteria such as P. acnes.6, 7
As would be expected with a membrane receptor designed to recognize foreign microbial invaders, the TLR2 signaling pathway is linked to the activation of NF-kB, with the subsequent release of inflammatory cytokines such as IL-1α, IL-6 and IL-8.6, 8 Intermediates in this signaling pathway between TLR2 and NF-kB appear to be MYD88, IRAK and TRAF6, although it also appears that cytokine production can occur via TLR2 activation using the p38/MAPK pathway, independent of NF-kB.9
Activation of TLR2 and the subsequent measurement of cytokine production using either cultured keratinocytes or sebocytes is a well-established model currently used to screen materials for anti-acne effects. While activation of TLR2 can be accomplished using cultured live P. acnes,9 heat-killed P. acnes or cell-free extracts of P. acnes,8 some labs my lack the equipment for microbiological culture or may be hesitant to introduce bacteria into an otherwise sterile cell culture facility. If this is the case, then TLR2 activation can be achieved using commercially available peptidoglycan agonists such as PGN-BS, PGN-EB, PGN-EK and PGN-SA.
In fact, the use of purified agonists may even be preferable to P. acnes since the concentrations of the TLR2 agonists can be more precisely controlled for experimental purposes. Regardless of the means to activate TLR2, the endpoint for the assay would involve the measure of cytokine release. This can easily be accomplished using ELISA-based methods, which provide effective measurements of how good any active would be at reducing the inflammation associated with P. acnes.
The interaction between P. acnes, skin cells and the pathogenesis of acne continues to be intensely researched.
In addition to TLR2 agonists, many compounds are available that can target specific parts of the TLR2 signaling pathway leading to inflammation. These include: TLR2 antagonists (sparstolonin B and CU-CPT22) or neutralizing antibodies (OPN-305); MYD88 inhibitors (ST2825 and NBP2-29328); IRAK inhibitors (AS 2444697); NF-kB inhibitors (JSH-23 and rolipram); as well as p38 MAPK inhibitors (SB 202190 and SB 203580). These compounds can provide a detailed analysis of whether given actives of interest may potentially impact TLR2 signaling—and where in they process they may decrease the release of inflammatory cytokines.
It should be noted that not all effects mediated by the TLR2 signaling pathway result in the release of inflammatory cytokines. Activation of the TLR2 pathway can also promote the release of antimicrobial proteins such as human β-defensin 4 from both sebocytes and keratinocytes, and also promote P. acnes uptake and digestion by sebocytes.7 Both of these responses promote a reduction in the P. acnes population in the infected area. Therefore, an ideal anti-acne active could preferentially reduce the excessive inflammatory response produced by TLR2 activation while also maintaining the release of antimicrobial proteins and uptake and destruction of P. acnes.
Sebum Production
In vitro models for sebocytes often employ immortalized versions of human sebocytes such as SZ95, SEB-1 and Seb-E6E7.11 However, the use of these cell lines can be restricted for certain applications or require a special licensing fee, which can prohibit their use in certain labs. Fortunately, in recent years, many commercial vendors for human cells have now started to offer primary cultures of normal human sebocytes. The growth of normal human sebocytes does require the use of specially treated cultureware, such as collagen or fibronectin coating of growth surfaces, but they are essentially simple cells to grow in a laboratory setting. These cells will typically can undergo a small, limited number of population doublings before requiring treatment with compounds such as insulin or IGF-1,12 adiponectin13 or LXRα, which induce lipid accumulation.14
It is during this lipid accumulation phase that actives can be screened to determine if they impact the lipid accumulation process, which can then be used as an index on the material's ability to inhibit sebum production. In sebocyte lipid accumulation assays, the sebocytes are often fixed at the end of the lipid accumulation phase and treated with Oil Red O, a common stain that marks accumulated lipids within the cell with a vivid red color. The Oil Red O staining can either be visualized microscopically in the fixed cells and/or recovered and measured using spectrophotometric-based methods to get a quantitative index of lipid accumulation. Both the visualization of Oil Red O and its quantitation can provide data on how well an active can reduce or inhibit lipid accumulation within the sebocytes, and its potential to reduce sebum production.
Keratinocyte Proliferation and P. acnes Reduction
Assays for cell proliferation and antibacterial activity are well-established. Cellular proliferation assays normally involve measuring either: the number of viable cells using an assay such as MTT, or DNA synthesis using an assay such as BrdU incorporation. To screen materials for anti-acne effects, keratinocyte proliferation is first stimulated using an acne-relevant stimulus such as androgens,15 insulin/IGF-116 or even fatty acids,17 then effects of the test material are measured to see if they attenuate a proliferative response. Antibacterial assays commonly use classic methods to determine the minimum inhibitory concentration (MIC) and minimum bactericidal concentration (MBC) of a compound versus P. acnes bacteria. This reveals whether the compound has antibacterial activity and the potential for use as an anti-acne active.15
It is little wonder why the skin care industry has a strong interest in developing products to counter the effects of acne.
Concluding Remarks
The anti-acne assays listed in this article are by no means comprehensive. The interactions between P. acnes bacteria, skin cells and the pathogenesis of acne are very complex and continue to be an intensely researched. However, these assays may provide a starting point from which to screen novel materials for their potential to benefit this all too common skin affliction.
References
- JK Tan and K Bhate, A global perspective on the epidemiology of acne, Brit J Derm 172 (supplement 1) 3–12 (2015)
- DD Lynn, T Umari, CA Dunnick and RP Dellavalle, The epidemiology of Acne vulgaris in late adolescence, Adolescent Health, Medicine and Therapeutics 7 13–25 (2016)
- CM Nguyen et al, The psychosocial impact of acne, vitiligo and psoriasis: A review, Clinical, Cosmetic and Investigational Derm 9 383–392 (2016)
- JH Yang et al, Seeking new acne treatment from natural products, devices and synthetic drug discovery, Dermato-Endocrinology 2(1) e1356520 1–6 (2017)
- U Ohto, Conservation and divergence of ligand recognition and signal transduction mechanisms in Toll-Like receptors, Chem and Pharma Bulletin 65 697–705 (2017)
- JL Selway, T Kurczab, T Kealey and K Langlands, Toll-like receptor 2 activation and comedogenesis: Implications for the pathogenesis of acne, BMC Dermatology 13 10 (2013)
- LD Hisaw et al, Antimicrobial activity of sebocytes agains P. acnes via Toll-like receptor 2 and lysosomal pathway, J Inves Derm 136 2098–2101 (2016)
- YC Huang, CH Yang, TT Li, CC Zouboulis and HC Hsu, Cell-free extracts of P. acnes stimulate cytokine production through the activation of p38 MAPK and Toll-like receptor in SZ95 sebocytes, Life Science 139 123–131 (2015)
- JM Kim, JE Choo, HJ Lee, KN Kim and SE Chang, Epidermal growth factor attenuated the expression of inflammatory cytokines in human epidermal keratinocytes exposed to P. acnes, Annals of Dermatology 30 54–63 (2018)
- YY Wang et al, Chlorin e6-mediated photodynamic therapy suppresses P. acnes-induced inflammatory response via NF-kB and MAPKs signaling pathway, PLoS ONE 12 e0170599 1–14 (2017)
- L Xia, CC Zouboulis and Q Ju, Culture of human sebocytes in vitro, Dermato-Endocrinology 1(2) 92–95 (2009)
- TM Smith, Z Cong, KL Gilliland, GA Clawson and DM Thiboutot, Insulin-like growth factor-1 induces lipid production in human SEB-1 sebocytes via sterol response element-binding protein-1, J Inves Derm 126, 1226–1232 (2006)
- YR Jung et al, Adiponectin signaling regulates lipid production in human sebocytes, PLoS ONE 12(1) e0169824 (2017)
- L Hong, MH Lee, TY Na, CC Zouboulis and MO Lee, LXRalpha enhances lipid synthesis in SZ95 sebocytes, J Inves Derm 128(5) 1266–72 (2008)
- CJ Lee, LG Chen, WL Liang and CC Wang, Multiple activities of Punica granatum linne against Acne vulgaris, Intl J Mol Sci 18 141 (2017)
- O Isard et al, P. Acnes activates the IGF-1/IGF-1R system in the epidermis and induces keratinocyte proliferation, J Inves Derm 131 59–66 (2011)
- BR Zhou, Palmitic acid induces production of proinflammatory cytokines IL-6, IL-1B and TNFa via a NF-kB-dependent mechanism in HaCaT keratinocytes, Mediators of Inflammation (2013)