The major function of skin, thanks to its stratum corneum location, is to prevent desiccation and protect against environmental hazards such as bacteria, chemicals and UV radiation. In addition to this primary role as a barrier, the skin is a metabolically active tissue that contains enzymes able to metabolize not only endogenous chemicals such as carbohydrates, lipids, proteins and steroid hormones, but also xenobiotics. Being the largest organ of the body, the skin is exposed both acutely and chronically to a wide variety of xenobiotics, either unintentionally through environmental pollutants or intentionally through drugs and cosmetics.
When xenobiotics contact the skin, lipophilic compounds are converted into more polar, water-soluble compounds. However, the role of this conversion in the absorption process is yet unknown, and understanding these mechanisms is important to understanding their impact on topical delivery. Therefore, the authors sought to develop a method to characterize these metabolic effects on absorption.
Metabolic Mechanisms
Developing an appropriate test first requires understanding the mechanisms of metabolism. As noted, when xenobiotics contact the skin, often the result is detoxification of the chemicals by converting lipophilic compounds into more polar, water-soluble compounds. This is accomplished through enzymatic reactions catalyzed by metabolizing enzymes present in the skin. Cytochrome P450 (P450 or CYP) is the key metabolic enzyme family, capable of metabolizing drugs and chemicals in hepatic and extrahepatic tissues, including skin.1–3 The special interest for CYP enzymes in skin is evident by the fact that most drugs used by practicing dermatologists are either substrate inducers or inhibitors of this enzyme family.1
In the skin, CYP enzymes act on various endogenous substrates including vitamins A and D, which are used widely for treating a variety of dermatological pathologies. In addition, many ingredients in cosmetics, toiletries and health care products, as well as a number of allergens, toxins and carcinogens to which the skin is exposed, serve as substrates for CYP. Data in the literature suggests that such metabolism could influence the absorption and diffusion of molecules that contact the skin.4 In fact, both the European Union Scientific Committee on Consumer Products (SCCP) and the Organization for Economic Cooperation and Development (OECD) skin absorption guidelines5, 6 recommend investigating the metabolism of lipophilic compounds, when expected.
However the role of cutaneous biotransformation in the absorption process is still a matter of scientific debate.5 Indeed, due to the difficulties in obtaining and maintaining viable skin, few studies are available on true skin metabolism, and the majority of the skin delivery experiments are conducted with frozen skin with inactivated biotransformation enzymes. Reconstructed human skin models offer long-term viability but exhibit a weak barrier function7 and although CYPs are detected by expression profiling, low CYP activity is detected in the reconstructed models tested.8
To overcome these limitations, studies were undertaken to develop a convenient short-term skin culture from domestic pig ears to characterize its metabolic capabilities. Pig skin, when sourced from slaughterhouses, provides a valuable alternative owing to its close resemblance to human skin from both histological and physiological viewpoints,9 and is recognized as an alternative model to animal testing.5, 6 Recent work on the validation of skin viability following UV irradiation10 showed that cultured pig ear skin displays good viability over a period of 48–72 hr. Therefore, this short-term culture model using pig ear skin was used to explore both skin delivery and phase I and II enzyme activities.
Materials and Methods
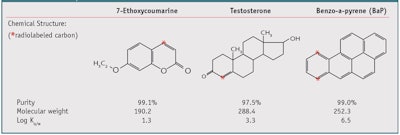
Three compounds, 7-ethoxycoumarine (7-EC),11 benzo(a)pyrene (BaP),11, 13 and testosterone,14 were selected both according to their log Ko/w, which reflects increasing lipophilicity (see Table 1), and potential to be metabolized in the skin. To determine how skin metabolism altered the dermal absorption of these compounds, all investigations compared their diffusion on both frozen pig skin and viable pig skin explants. The key published results11–14 are summarized and reviewed here. The most hydrophilic molecule of the three is 7-EC; testosterone is a model molecule in skin delivery recommended by the OECD6 and is known to be extensively metabolized by phase I enzymes; and BaP is a lipophilic compound, also known to be metabolized through CYP dependent pathways and phase II enzymes. 3, 4
Extensive details for preparing the skin explants are described by Jacques et al.11 Briefly, skin organ culture was developed from the ears of domestic pigs obtained from a local slaughterhouse. After cleaning and shaving, the skin was excised, dermatomed at a thickness of 500 μm and punched into 28-mm diameter discs. Skin punches were seeded dermal side-down in polycarbonate inserts and placed in a 6-well plate prefilled with 1.5 mL culture medium (DMEM) at 37°C in a 5% CO2 air incubator (see Figure 1). As noted, the influence of skin metabolism on dermal absorption was investigated by comparing the compound diffusion in viable explants with the corresponding skin preparation that had previously been frozen for two months at -20°C.
The design of the topical application of the test molecules on the skin models for 72 hr and compartmental analysis also are properly described by Jacques et al.11–14 but briefly, skin explants were exposed to different doses of radio-labeled 7-EC, testosterone and BaP. All incubations were carried out in triplicate. Culture media, collected at 24 hr, 48 hr and 72 hr, were stored at -20°C until analysis. Skin surfaces, tissue culture inserts and wells were washed twice with acetonitrile or methanol, according to the physicochemical properties of the compound studied. Compounds and metabolites were extracted from skin after homogenization in a methanol/phosphate buffer and centrifugated. Radioactivity in culture media, skin extracts and washing solutions was quantified by scintillation counting. Analyses were performed by radio high-performance liquid chromatography (radio-HPLC), liquid chromatography–mass spectrometry (LC-MS), gas chromatography-mass spectroscopy (GC-MS) and nuclear magnetic resonance (NMR).
Results
For all the experiments carried out with fresh or frozen skin, more than 90% of the applied radioactivity was recovered in the culture media, as measured every 24 hr for 72 hr, and all other compartments, i.e., skin, skin surface, wells and inserts, and washing solutions, which complies with the OECD guideline requirements.6
7-EC in fresh and frozen skin:1 After 72 hr, all but approximately 1% of the radioactivity was absorbed into the skin surface. The skin itself contained approximately 10% of the applied radioactivity. The majority of radioactivity was located in the culture media in a similar dose as was applied to skin. The diffusion of 7-EC was similar between fresh (74 ± 4%) and frozen skin (78 ± 3%). As expected, from frozen skin samples, no metabolite was found in any skin compartment. In viable skin, however, significant amounts of metabolized 7-EC were detected, mainly in culture media. For instance, 48 hr after a 10-nmoles dose of 7-EC was applied, 25% of the radioactivity present in the culture media, corresponding to 17% of applied radioactivity, was associated with 7-EC metabolites.11 Three metabolites were detected by radio-HPLC: the 7-hydroxycoumarin (OH–C) and corresponding glucuronyl (G–O–C) and sulphate (S–O–C) conjugates, respectively.
Testosterone in fresh and frozen skin:1 For testosterone, the entire radioactivity applied permeated into the skin after 72 hr. The nonabsorbed radioactivity was slightly higher for frozen skin but insignificantly so (see Figure 2). In the skin, the percentage of radioactivity recovered increased with higher quantities applied to skin. For example, the applied radioactivity was found, in skin, to increase from 10 ± 1% with 50 nmoles testosterone, to 32 ± 5% of 800 nmoles testosterone.4 The percentage of radioactivity recovered in the culture media was significantly different between fresh and frozen skin, especially at the lower doses. For instance, the diffusion was approximately 80 ± 5% in fresh skin, and 60 ± 3% in frozen skin with a 200 nmoles dose (see Figure 2).
Moreover, in frozen skin, 60% of the radioactivity found in the culture media was only the parent compound. In fresh skin, the parent compound represented only 3% and the other 81%, metabolites. Using radio-HPLC and GC-MS, the following phase I metabolites were detected in the culture medium: androstenedione; 5α-androstane-3,17-dione; androsterone; epiandrosterone; Δ6-testo; OH-Δ4-diones; OH-testosterone; and testosterone oxidated at the 7α, 6β, 16α positions. Whatever dose was applied to skin, most of the parent compound was metabolized just after penetration, meaning that skin was able to metabolize large amounts of steroids. Phase I enzymes involved in the biotransformation of testosterone were not saturated even at 800 nmoles, the highest concentration of testosterone applied.1
BaP in fresh and frozen skin:12, 13 BaP was the only molecule where the fraction of radioactivity was absorbed in a dose-dependent manner both in frozen and fresh skin. In skin itself, significantly higher percentages of radioactivity were recovered in frozen skin than fresh skin. In addition, the diffusion of BaP in frozen skin, i.e., the percent of radioactivity in culture media, was very low compared to fresh skin, regardless of the BaP dose applied (see Figure 3).
As for the previous molecules tested, only the parent compound was found in the culture media when applied in frozen skin. An insignificant amount of parent compound was found in this compartment between fresh (4 ± 1%) and frozen skin explants (5 ± 7%). However, a significantly higher amount of metabolites was detected in the culture media when BaP was applied on fresh skin. LC-MS and NMR identified the presence of nine groups of metabolites.12 BaP-diols, BaP-tetrols, BaP-catechols, BaP-diones, BaP-OH isomers and glucuronyl and sulfate conjugates were the major compounds formed in the pig ear skin model. For these conjugates, enzymatic kinetic curves showed a saturation occurring around 200 nmoles of BaP applied on the skin explants.13
Discussion
Viable skin and delivery: As described, to determine how and to what extent skin metabolism alters the skin delivery of xenobiotics, the diffusion of three compounds with different physicochemical properties were studied on a pig ear skin model comparing frozen and fresh skin. For the three compounds, freezing the skin inactivated the biotransformation enzymes and only the parent compound was recovered in the different skin compartments. The amount that diffused into the culture media, i.e., the receptor compartment, decreased according the log Ko/w of the compounds tested (see Figure 4).
However, for the less lipophilic compounds, no significant difference in skin diffusion of 7-EC was observed in frozen or fresh skin. Due to its low molecular weight and a log Ko/w of 1.3, 7-EC diffused quickly through the skin and did not remain in contact with biotransformation enzymes. Therefore, the rate of metabolism was low, ranging from 17% at 10 nmoles to 4% at 400 nmoles of 7-EC.11 For testosterone, the percentage of radioactivity recovered in the culture media was significantly different with approximately 60% and 80% of the dose applied in frozen and fresh skin, respectively. In frozen skin, the 60% was the parent compound only. In fresh skin, only 3% was testosterone, together with approximately 78% of testosterone metabolites (see Figure 4).
Regarding the most lipophilic molecule, BaP penetrated easily into the lipidic layers of the stratum corneum but diffused in very small amounts through the hydrophilic epidermis and dermis. In frozen skin, after 72 hr, only 4% of the applied radioactivity was found in the culture media. In fresh skin, about 30% of the radioactivity was detected in the culture media; 5% was the parent compound and the other 25% was BaP metabolites (see Figure 4). These are remarkable results, confirming that skin metabolism strongly alters the skin diffusion of lipophilic compounds.
Viable skin and metabolic capacities: Mukhtar published an extensive review1 on CYP and their related functions in the skin. Most of the known CYP are expressed in the skin. According to the different metabolites identified from the three molecules tested, the following phase I enzymes were identified in the viable pig ear skin model: CYP1A1 and A2; CYP1B1; CYP2C; CYP3A; CYP19A; and 7-ethoxycoumarin-O-deethylase, also known as ECOD. According to Katayar et al.,15 CYP are mainly located in the epidermis. CYP1A1 is primarily localized in the basal cell layer of the epidermis, whereas CYP1B1 is localized in epidermal cells other than the basal cell layer. The authors previously suggested15 this different localization of CYP1A1 and CYP1B1 in the epidermis may be related to keratinocyte differentiation. The phase II enzymes identified were glucuronyl-S-transferase; UGT 1A and 2B; and sulfo-tranferase, SULT 1A, 1B and 1E; also mainly localized in the epidermis.
Based on the findings, the viable pig ear skin model exhibits both a good barrier function and functional key phase I and phase II enzymes. Metabolism still occurs even after 72 hr. The viable pig ear skin model represents a suitable alternative to human skin to study both the delivery and metabolism of lipophilic compounds in short-term experiments, either to test single topical applications or even to simulate short chronic applications.
The described studies give a better understanding of what happens to chemicals when they come into contact with skin. Accordingly, the stratum corneum acts as the first physical barrier, blocking the delivery of molecules having a molecular weight above 500 Da16 and most hydrophilic ones. The small lipophilic compounds are solubilized into the lipidic layers of the stratum corneum, thus creating a reservoir. According to the first Fick’s Law, a gradient of concentration appears, creating a driving force for slow delivery into the viable epidermis. Being in contact with the CYP enzymes, these compounds are therefore biotransformed into hydrophilic ones to ensure quick transfer into the bloodstream, and then excreted. Accordingly, researchers can consider that skin as acting first as a barrier, via the stratum corneum, but when lipophilic xenobiotics bypass this barrier, the second line of defense, located in the viable epidermis, metabolizes these compounds to ensure quick excretion out of the body, the skin acting then as a peripheral liver.
Conclusion
These findings raise many questions about how lipophilic compounds from cosmetic formulations are really delivered and metabolized. The commonly used anti-aging ingredient retinol has a similar lipophilicity to BaP, and therefore its skin delivery is low. The fraction delivered into the skin is mostly esterified into a storage form. A very small fraction is biotransformed into retinoic acid, which is then catabolized by CYP 26.17 However, considering these findings, do researchers really know how retinol is delivered and biotransformed in the skin? Is the long-term topical application of retinol inducing higher expressions of CYP26, the catabolic enzyme for retinoic acid? And what is the best skin care routine to sustain an optimal anti-aging treatment? Many of these questions could apply to several lipophilic cosmetic ingredients used daily in cosmetic formulations.
This brings cosmetic research closer and closer to drug research with a typical absorption, diffusion, metabolism and excretion, or ADME, approach. This will sooner or later impact cosmetic regulations, although it also opens a widely amazing field of investigation for further exploration, in order to improve the safety and efficacy of topically active ingredients in particular, and all cosmetics applied in general.
References
Send e-mail to [email protected].
- C Jacques, E Perdu, C Dorio, D Bacqueville, A Mavon and D Zalko, Percutaneous absorption and metabolism of [14C]-ethoxycoumarin in a pig ear skin model, Toxicol In Vitro 24, 1426–1434 (2010)
- C Jacques, EL Jamin, E Perdu, H Duplan, A Mavon, D Zalko and L Debrauwer, Characterization of B(a)P metabolites formed in an ex vivo pig skin model using three complementary analytical methods, Anal Bioanal Chem 396(5) 1691–701 (2010)
- C Jacques et al, Disposition and biotransformation of 14C-Benzo(a)pyrene in a pig ear skin model: Ex vivo and in vitro approaches, Toxicol Lett 199(1)22–33 (2010)
- C Jacques et al, Disposition and biotransformation of 14C-testosterone in an ex vivo pig ear skin model and in vitro approaches, J Controlled Released (2012) (submitted)
- N Ahmad and H Mukhtar, Cytochrome P450: A target for drug development for skin diseases, J Invest Dermatol 123 417–425 (2004)
- HF Merk, J Abel, JM Baron and J Krutmann, Molecular pathways in dermatotoxicology, Toxicol Appl Pharmacol 195 267–277 (2004)
- F Oesch, E Fabian, B Oesch-Bartlomowicz, C Werner and R Landsiedel, Drug metabolizing enzymes in the skin of man, rat and pig, Drug Metab Rev 39 659–698 (2007)
- JE Storm, SW Collier, RF Stewart and RL Bronaugh, Metabolism of xenobiotics during percutaneous penetration: Role of absorption rate and cutaneous enzyme activity, Fundam Appl Toxicol 15 132–141 (1990)
- SCCS, Basic criteria for the in vitro assessment of dermal absorption of cosmetic ingredients, adopted by the Scientific Committee of Consumer Products during the 7th plenary of 22 June 2010, SCCS/1538/10 (2010)
- OECD, Guidance notes on dermal absorption, draft (Oct 22, 2010)
- N Garcia, O Doucet, M Bayer, D Fouchard, L Zastrow and JP Marty, Characterization of the barrier function in a reconstituted human epidermis cultivated in chemically defined medium, Int J Cosmet Sci 24, 25–34 (2002)
- C Jäckh, V Blatz, E Fabian, K Guth, B van Ravenzwaay, K Reisinger and R Landsiedel, Characterization of enzyme activities of Cytochrome P450 enzymes, Flavin-dependent monooxygenases, N-acetyltransferases and UDP-glucuronyltransferases in human reconstructed epidermis and full-thickness skin models, Toxicology in Vitro 25 1209–1214 (2011)
- NA Monteiro-Riviere, AO Inman, BM Barlow and RE Baynes, Dermatotoxicity of cutting fluid mixtures: In vitro and in vivo studies, Cutaneous Ocular Toxicol 25, 235–247 (2006)
- D Bacqueville and A Mavon, Caspase-3 activation and DNA damage in pig skin organ culture after solar irradiation, Photochem Photobiol 84 1164–1171 (2008)
- SK Katiyar, MS Matsui and H Mukhtar, Ultraviolet-B exposure of human skin induces cytochromes P450 1A1 and 1B1, J Invest Dermatol 114 328–333 (2000)
- JD Bosand and MM Meinardi, The 500 Dalton rule for the skin penetration of chemical compounds and drugs, Exp Dermatol 9(3) 165–169 (2000)
- E Pavez Loriè, H Li A Vahlquist and H Törmä, The involvement of cytochrome p450 (CYP) 26 in the retinoic acid metabolism of human epidermal keratinocytes, Biochim Biophys Acta 1791(3) 220–228 (2009)





!['We believe [Byome Derma] will redefine how products are tested, recommended and marketed, moving the industry away from intuition or influence, toward evidence-based personalization.' Pictured: Byome Labs Team](https://img.cosmeticsandtoiletries.com/mindful/allured/workspaces/default/uploads/2025/08/byome-labs-group-photo.AKivj2669s.jpg?auto=format%2Ccompress&crop=focalpoint&fit=crop&fp-x=0.49&fp-y=0.5&fp-z=1&h=191&q=70&w=340)



