(continued from Part I)
Materials and Methods
Materials: As noted, a blend HR and EL (HREL)a was developed for the described studies. The HR used for this blend has a purity of at least 99% and is practically devoid of free resorcinol (< 0.05%)b. The EL used has a linoleic acid content of at least 70%c.
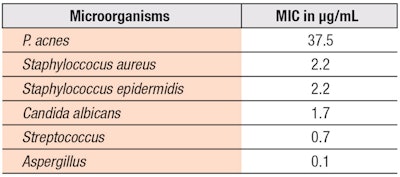
Antimicrobial efficacy of HR and HREL: Broad anti-bacterial and antifungal activities are also desired for anti-acne treatments since, as noted, affected skin has much higher levels of Staphylococcus and candida.22 An antimicrobial test for this study was carried out as per the Category 2, USP Pharmacopeia’s Compendia Products.44
Transcription regulatory activity of NF-κB: This assay followed the method described by Yang et al.45 HREL was first dissolved in dimethyl sulfoxide (DMSO) and further diluted into various concentrations with cell media, for a total 1% DMSO in each sample; media containing 1% DMSO only served as vehicle controls. The murine myoblast C2C12 cells, transfected with an NFκB luciferase reporter gene, were treated with the above cell media with different concentrations of product and fixed quantity of TNFα. The transcription regulatory activity of NFκB was quantified by adding luciferase assay reagent to each well and the luminance reading was then recorded.
Quantification of NF-κB protein: In a separate assay,46 human 293T cells were cultured in DMEM medium supplemented with 10% fetal bovine serum, L-glutamine and penicillin-streptomycin. Cells were seeded (1 × 105/mL) to a 24-well plate and cultured overnight. The culture medium was replaced by serum-free medium for 4 hr to “starve off” the serum. TNFα (100 ng/mL) and testing sample extracts were then added at a concentration of 1 mg/mL into each well, and cells were cultured at 37°C with CO2 for 1 hr.
Whole cell proteins were extracted and levels of NF-κB were measured using an ELISA kit. The levels of NF-κB protein of each sample were calculated against a standard curve, constructed using recombinant NF-κB standard.
Effects on PIH: Chaudhuri previously reported27 that HR is also effective in reducing hyper-pigmented spots without affecting the surrounding areas. Eighteen volunteers between the ages of 42 and 60 applied a 1% HR lotion twice daily in an amount sufficient to cover their upper arm, specifically targeting hyper-pigmented spots. The treated skin of each volunteer was evaluated and the percent reduction in pigmentation was determined using ITA0.
Anti-acne clinical study: A six-week clinical study of 10 subjects, ages 21.30 ± 4.54, was conducted including: five male and five female Caucasian (nine) and Hispanic (one) participants. Fitzpatrick Types included: II (two), III (six) and IV (two); all subjects presented with mild acne according to an expert grader—specifically: ≥ 5 and ≤ 20 total inflammatory and non-inflammatory lesions, and ≥ 3 inflammatory lesions. The subjects applied a 3% HREL lotion (see Formula 1) twice daily for the duration of the study.
Objective assessments of skin tolerance including dryness, erythema and edema, and subjective assessments of stinging, itching, tingling and burning all indicated the formula was well-tolerated. Photographs were taken of acne lesions, PIH and pores for image analyses. In addition, subjects completed a questionnaire and experts graded subjects regarding the effects of treatment compared with baseline for: 1) total acne lesions, 2) inflammatory acne lesions (whiteheads), 3) non-inflammatory acne lesions (blackheads), 4) PIH and 5) the overall texture/appearance of skin.
Results and Discussion
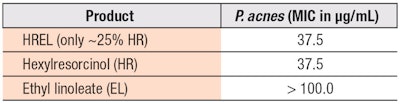
Antibacterial/antifungal efficacy of HR and HREL: HR indeed was found to be a broad-spectrum antibacterial/antifungal agent (see Table 1). In addition, it showed synergy when blended with EL, which has no antibacterial or antifungal activity at the dose tested (see Table 2).27
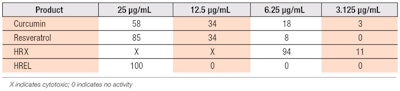
Transcription regulatory activity of NF-κB and quantification of NF-κB protein: Using two different methods, HR was shown to be a potent inhibitor of NF-κB, and as Table 3 shows, was even superior to the well-known inhibitors curcumin (see Figure 4) and resveratrol (see Figure 5). This inhibitory effect of the HR remained intact in the HREL blend (see Figure 6 and Table 3).
Effects on PIH: Previous studies showed that HR is an effective compound in reducing hyper-pigmented spots without affecting the surrounding areas.27 Furthermore, it stimulated endogenous antioxidant defenses, specifically glutathione, glutathione peroxidase and glutathione reductase.27 When compared with coloration on day zero (pre-application), the treated hyper-pigmented spots showed a statistically significant (p < 0.05) reduction of 39% and 60% in pigmentation at four and eight weeks, respectively (see Figure 7). On the other hand, the treated area of the skin surrounding the hyper-pigmented spots showed only marginal changes with no statistical significance when compared to day zero (pre-application).
Clinical study, subjective parameters: Subjective questionnaires were completed by panelists (and experts) based on three subjective parameters: pigmented spots, skin tone and roughness/dryness using a scale of 0 = no improvement; 1 = minimal; 2 = moderate; 3 = good and 4 = excellent improvement. Results indicated subjects had an overall positive response to the test product (see Figure 8 and Figure 9), i.e., 3% HREL lotion (Formula 1), as far as effectiveness in reducing the appearance of inflammatory and non-inflammatory lesions and PIH, and improving the overall texture/appearance of skin. After six weeks of treatment, all subjects saw a significant reduction in erythema (p = 0.015), with no incidence of worsening in any tolerance parameters, compared with baseline.
Clinical study, objective parameters: Clinical grading findings indicating a statistically significant reduction (p < 0.05) in acne lesions after three and six weeks of product use (3% HREL lotion; see Figure 10). Additionally, image analysis (see Figure 11) revealed a significant improvement in PIH as well as a reduction in average diameter (size) of pores and pore count after six weeks of product use. Note that the three-week data for PIH, average pore and pore counts was statistically not significant; six-week results for all four parameters, however, was significant at p < 0.05. Figure 12, Figure 13 and Figure 14 show subjects’ skin before (a) and after (b) treatment with 3% HREL lotion treatment for six weeks.
Formulation Considerations
HREL represents a new blend of well-known ingredients that combines several mechanisms of action to clear away acne. Furthermore, it is theorized that by combining it with other anti-acne ingredients, described next, additional improvements in anti-acne properties can be achieved.
Salicylic acid, 2%: Salicylic acid helps to correct the abnormal shedding of skin cells and unclogs pores to resolve and prevent lesions.
Bakuchiol, 0.25%: This ingredient can inhibit the formation of squalene peroxide, which promotes acne and roughens and wrinkles skin.47 Bakuchiol is an excellent lipid peroxidation inhibitor (IC50 = 0.61; IC100 = 1.46 µg/mL; squalene as a substrate) that is significantly more effective than natural tocopherol (IC50 = 30 µg/mL)48 and also has broad-spectrum anti-aging benefits.16
Niacinamide, 2%: This ingredient provides potent anti-inflammatory activity without the risk of inducing bacterial resistance.49
Conclusion
By extensively analyzing the various mechanistic pathways of acne, these authors describe the development of an ingredient blend based on hexylresorcinol (HR) and ethyl linoleate (EL) to treat acne. After six weeks of treatment with an HREL-containing product, 10 subjects experienced significantly reduced inflammatory and non-inflammatory acne lesions, PIH, and average pore diameters and pore counts, as well as overall improvements to the texture and appearance of their skin.
Significant reductions in erythema also were observed, with no evidence of worsening in any tolerance attributes, compared with the baseline. Interestingly, HREL was found to be more effective in inhibiting transcription regulatory activity of NFκ-B, compared with known inhibitors curcumin and resveratrol. While effective anti-acne products could be developed based on HREL alone, the authors note the appropriate selection of co-actives could theoretically prove even more effective.
References
- E Hollander and CM Wong, Body dysmorphic disorder, pathological gambling and sexual compulsions, J Clin Psychiatry 56 suppl 4 7-12; discussion 13 (1995)
- E Ingham, EA Eady, CE Goodwin, JH Cove and WJ Cunliffe, Pro-inflammatory levels of interleukin-1 alpha-like bioactivity are present in the majority of open comedones in acne vulgaris, J Invest Dermatol 98 895–901 (1992)
- B Vowels, S Yang and J Leyden, Induction of pro-inflammatory cytokines by a soluble factor of Propionibacterium acnes: Implications for chronic inflammatory acne, Infect Immun 63 3158–3165 (1995)
- R Marples, J Leyden, R Stewart, O Mills and A Kligman, The skin microflora in acne vulgaris, J Invest Dermatol 62 37–41 (1974); G Webster and J Leyden, Characterization of serum-independent polymorphonuclear leukocyte chemotactic factors produced by P. acnes, Inflammation 4 261–269 (1980)
- CC Zouboulis, Acne and sebaceous gland function, Clin Dermatol 22 360–366 (2005)
- Q et al, Propionibacterium acnes-induced IL-8 production may be mediated by NF-kappaB activation in human monocytes, J Dermatol Sci 29(2) 97-103 (2002)
- S Kang, S Cho, JH Chung, C Hammerberg, GJ Fisher and JJ Voorhees, Inflammation and extracellular matrix degradation mediated by activated transcription factors Nuclear Factor-κB and activator protein-1 in inflammatory acne lesions in vivo, Am J Pathol 166(6) 1691–1699 (2005)
- S Kaur, T Oddos, S Tucker-Samaras and MD Southall, Regulation of DNA repair process by the pro-inflammatory NF-k-B pathway, Intech (2013) http://dx.doi.org/10.5772/54341
- EC Davis and VD Callender, A review of acne in ethnic skin: Pathogenesis, clinical manifestations and management strategies, J Clin Aesthet Dermatol 3(4) 24–38 (2010)
- E Davis E and Callender VD, A Review of the Epidemiology, clinical features and treatment options in skin of color, J Clin Aesthet Dermatol 3(7) 20–31 (2010)
- SC Taylor et al, Acne vulgaris in skin of color, J Am Acad Dermatol 46 (2 Suppl) S98–S106 (2002)
- VD Callender, Acne in ethnic skin: Special considerations for therapy, Dermatol Ther 17 184–195 (2004)
- S Tsao, J Dover, K Arndt and M Kaminer, Scar management: Keloid, hypertrophic, atrophic and acne scars, Semin Cutan Med Surg 21 46–75 (2002); R Hirsch and A Lewis, Treatment of acne scarring, Semin Cutan Med Surg 20 190–198 (2001)
- E Araviiskaia and B Dreno, The role of topical dermocosmetics in acne vulgaris, J Eur Acad Dermatol Venereol doi: 10.1111/jdv.13579
- RK Chaudhuri, Bakuchiol: A retinol-like functional compound modulating multiple retinol and non-retinol targets, in RK Sivamani, J Jagdeo, P Elsner and HI Maibach, eds, Cosmeceuticals and Active Cosmetics, 3rd edn, Francis & Taylor, Boca Raton ch 1 1-18 (2015)
- RK Chaudhuri and K Bojanowski, Bakuchiol: A retinol-like functional compound revealed by gene expression profiling and clinically proven to have anti-aging effects, Intl J Cos Sci 36(3) 221-230 (2014)
- C Letawe, M Boone and GE Piecard, Digital image analysis of the effect of topically applied linoleic acid on acne microcomedones, Clin Exp Dermatol 23(2) 56-58 (1998)
- ME Stewart, MO Grahek , LS Cambier, PW Wertz and DT Downing, Dilutional effect of increased sebaceous gland activity on the proportion of linoleic acid in sebaceous wax esters and in epidermal acylceramides, J Invest Dermatol 87(6) 733-6 (1986)
- CC Zouboulis et al, Establishment and characterization of an immortalized human sebaceous gland cell line (SZ95), J Invest Dermatol 113 1011–1020 (1999)
- D Thiboutot et al, Human skin is a steroidogenic tissue: Steroidogenic enzymes and cofactors are expressed in epidermis, normal sebocytes and an immortalized sebocyte cell line (SEB-1), J Invest Dermatol 120 905–914 (2003)
- http://content.time.com/time/magazine/article/0,9171,719908,00.html (Accessed Jul 20, 2016)
- S Nishijima, I Kurokawa, N Katoh and K Watanabe, The bacteriology of acne vulgaris and antimicrobial susceptibility of Propionibacterium acnes and Staphylococcus epidermidis isolated from acne lesions, J Dermatol 5 318-323 (2000)
- RS Chhabra et al, Inhibition of some spontaneous tumors by 4-hexylresorcinol in F344/N rate and B6C3F1 mice, Fundam Appl Toxicol 11 685–690 (1988)
- V Buchholz et al, Topical antiseptics for the treatment of sore throat block voltage-gated neuronal sodium channels in a local anesthetic-like manner, Naunyn Schmiedebergs Arch Pharmacol 380(2) 161-168 (2009)
- AB Ross, A Kamal-Eldin and PD Aman, Alkylresorcinols: Absorption, bioactivities and possible use as biomarkers of whole-grain wheat- and rye-rich foods, Nutrition Rev 62(3) 81-95 (2004) and references cited therein
- A Kozubek and JHP Tyman, Resorcinolic lipids, the natural nonisoprenoid phenolic amphiphiles and their biological activity, Chem Rev 99 1-25 (1999)
- Ibid Ref 15, pp 73-83
- BL Hungund BL, S Zheng and AI Barkai, Turnover of ethyl-linoleate in rat plasma and its distribution in various organs, Alcohol Clin Exp Res 19(2) 374-377 (1995)
- A Hashimoto et al, Effect of the dietary alpha-linolenate/linoleate balance on leukotriene production and histamine release in rats, Prostaglandins 36 3-15 (1988)
- E Soyland et al, Effect of dietary supplementation with very-long-chain n-3 fatty acids in patients with psoriasis, N Engl J Med 328 1812-1816 (1993)
- NK Lowe and PR Dequoy, Linoleic acid effects on epidermal DNA synthesis and cutaneous prostaglandin levels in essential fatty acid deficiency, J Invest Dermatol 70(4) 200-203 (1978)
- C Prottery, PJ Hartop and M Press M, Correction of the cutaneous manifestations of essential fatty acid deficinecy in man by application of sunflower seed oil to the skin, J Invest Dermatol 64(4) 228-234 (1975)
- J Vicanova, AM Weerheim, JA Kempenaar and M Ponec, Incorporation of linoleic acid by cultured human keratinocytes, Arch Dermatol Res 291(7–8) 405–412 (1999)
- PM Elias, BE Brown and VA Ziboh, The permeability barrier in essential fatty acid deficiency: Evidence for a direct role for linoleic acid in barrier function, J Invest Dermatol 74(4) 230-233 (1980)
- G Imokawa, S Akasaki, Y Minematsu and M Kawai, Importance of intercellular lipids in water-retention properties of the stratum corneum: Induction and recovery study of surfactant dry skin, Arch Dermatol Res 281(1) 45-51 (1989)
- JW Fluhr, J Kao, M Jain, SK Ahn, KR Feingold and PM Elias, Generation of free fatty acids from phospholipids regulates stratum corneum acidification and integrity, J Invest Dermatol 117(1) 44-51 (2001)
- E Makrantonaski, R Ganceviciene and C Zouboulis, An update on the role of the sebaceous gland in the pathogenesis of acne, Dermatoendocrinol 3(1) 41–49 (2011)
- G Zhao et al, Anti-inflammatory effects of polyunsaturated fatty acids in THP-1 cells, Biochem Biophys Res Commun 336(3) 909-917 (2005)
- H Ando, A Ryu, A Hashimoto, M Oka and M Ichihashi, Linoleic acid and α-linolenic acid lightens ultraviolet-induced hyperpigmentation of the skin, Arch Dermatol Res 290 375-381 (1998)
- H Ando et al, Possible involvement of proteolytic degradation of tyrosinase in the regulatory effect of fatty acids on melanogenesis, J Lipid Res 40 1312–1316 (1999)
- M Ottaviani, E Camera and M Picardo, Lipid mediator in acne, Mediators of Inflammation, Article ID 858176 (2010)
- S Huh et al, Melanogenesis inhibitory effect of fatty acid alkyl esters isolated from Oxalis triangularis, Biol Pharm Bull 33(7) 1242-1245 (2010)
- A Charakida, M Charakida and AC Chu, Double-blind, randomized, placebo-controlled study of a lotion containing triethyl citrate and ethyl linoleate in the treatment of acne vulgaris, Brit J Dermatol 157(3) 569-574 (2007)
- webmd.com/skin-problems-and-treatments/acne/understanding-acne-treatment (Accessed July 20, 2016)
- J Yang, B Ou, ML Wise and Y Chu, In vitro total antioxidant capacity and anti-inflammatory activity of three common oat-derived avenanthramides, Food Chemistry 160 338-345 (2014)
- www.activemotif.com/catalog/216/transam-nf%CE%BAb-p50-p52-p65-family-kits (Accessed Jul 20, 2016)
- K Chiba, T Sone, K Kawakami and M Onoue, Skin roughness and wrinkle formation induced by repeated application of squalene monohydroperoxide to the hairless mouse, Exper Dermatol 8 471–479 (1999)
- RK Chaudhuri RK and B Ou, Bakuchiol to stabilize retinol and polyunsaturated lipids, Cosm & Toil 130 64-75 (2015)
- AR Shalita, JG Smith, LC Parish, MS Sofman and DK Chaker, Topical nicotinamide compared with clindamycin gel in the treatment of inelammatory acne vulgaris, Internl J Dermatol 34(6) 434-437 (1995)
~ Cosmetics & Toiletries ~